Connect With Us
Bunions
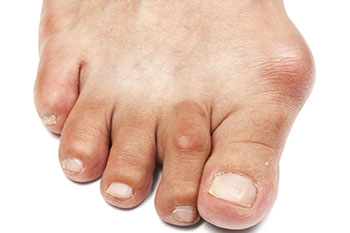
A bunion is a bony, painful swelling that is often formed on the first joint of the big toe. Bunions can be extremely painful due to the weight of all your body resting on it each time you take a step. Everyday activities, such as walking and wearing shoes, can cause you extreme discomfort if you have a bunion.
Reasons that a person may develop a bunion can vary. Some patients may form bunions due to genetic factors, complications with arthritis, or a weak foot structure. General aging can also play a role in the formation of a bunion.
If you have a bunion, you may notice a bony bump on your big toe, experience swelling and redness, and the area may feel tender to the touch. To help alleviate the pain that often comes with having a bunion, it’s suggested to maintain a healthy weight to help lessen the pressure on your toe, practice both heating and icing the affected area, wear wide-fitting shoes wear to leave plenty of space for your toes and to minimize rubbing, and look into shoe inserts that can help position your foot correctly.
Because bunions can result in other painful foot problems, such as hammertoes and bursitis, we recommend that you meet with a podiatrist for a professional diagnosis and for information regarding all your treatment options.
Lapiplasty
Bunions are complex deformities that can be very painful. Emmanuel Bustos, DPM is pleased to offer a new, patented treatment for bunion correction-Lapiplasty® 3D Bunion Correction.
What is Lapiplasty® 3D Bunion Correction?
Lapiplasty® 3D Bunion Correction is an advanced surgical procedure that corrects a bunion by rotating the entire deviated bone back into its normal anatomical position. This is done using specially-designed instrumentation, naturally straightening your toe and removing the “bump” and associated pain. Innovative plating technology is used to permanently secure the unstable joint. Most patients are able to walk within days of surgery. No cast is required; allowing patients to get back to the shoe wear of their choice and activities quickly.


Lapiplasty® Patented Titanium
The Lapiplasty® Procedure utilizes two low-profile (petite), anatomically-shaped titanium plates to permanently secure the unstable foundation of your corrected bunion. This provides buttressing on multiple planes and allows you to walk within days of surgery. Think of this in terms of how a basketball player might hold a basketball. When a player tightly grips the ball with both hands, the ball is held more securely than if only one hand is used.



What Should I Expect In Terms Of Recovery?
The patented titanium plating technology used with the Lapiplasty® Procedure enables patients to bear weight on their foot early. The ability to do so can dramatically improve your recovery process, allowing you to walk up to 6-8 weeks earlier than with the more traditional Lapidus approach (which was previously the only option for addressing the unstable joint).
Being able to walk in a surgical boot, as opposed to being completely non-weight bearing (in a cast with scooter or crutches) for 6-8 weeks, means that you will be getting back to a better quality of life faster; may return to most occupations more quickly; and will be less inconvenienced by bunion surgery.
Frequently Asked Questions
Below are some questions patients commonly ask and their respective answers:
How long does it take to recover from a Lapiplasty® Procedure?
Patients are typically walking within days of surgery. Patients can return to most occupations within days to a couple of weeks, wearing a surgical boot. Within six weeks, you can expect to be walking in comfortable shoes such as tennis shoes, however you should not plan on any high-impact activities for 3-4 months. Short shopping trips and leisurely strolls are examples of the types of activities that should be fine at this point. Around the 4-month mark post-op, you should be able to return to most activities and most shoe wear.
Can I wear fashionable shoes again?
The Lapiplasty® Procedure allows most patients to return to their desired shoes. Of course, some fashionable shoes can be painful (even with a normal foot!), so results can vary from person to person and shoe to shoe.
Can I play sports after the Lapiplasty® Procedure?
Yes, there are no permanent activity limitations after the Lapiplasty® Procedure. Most patients are able to return to most activities after the bones have completely healed at approximately 4 months.
Can the Lapiplasty® Procedure be performed on someone who has previously had traditional surgery?
Yes, the Lapiplasty® Procedure is an option that can be utilized by your doctor when a revision is required. Even if previously treated, patients can experience the same benefits from Lapiplasty® – with a permanently secured foundational joint this time around.
I’ve heard the term “reproducible” used when describing the Lapiplasty® Procedure. What does that mean?
“Reproducible” means that a procedure is easily repeatable with expected results. The Lapiplasty® Procedure utilizes precision, patented instrumentation designed to take the guesswork and “eyeballing” out of bunion surgery; helping ensure your surgeon can get reliable results over and over.
Can the Lapiplasty® Procedure be performed as an outpatient procedure & how long does it last?
Yes, Lapiplasty® surgeries are performed as outpatient procedures. Typically, the surgery will last just under an hour. If your doctor is performing any additional procedures at the same time, the surgery may take longer.
The Lapiplasty Procedure patient education brochure
 Lapiplasty® 3D Bunion Correction Brochure
Lapiplasty® 3D Bunion Correction Brochure
 Lapiplasty® 3D Bunion Correction
Lapiplasty® 3D Bunion Correction
 Lapiplasty® 3D Bunion Correction Before and After
Lapiplasty® 3D Bunion Correction Before and After
Minimally Invasive Surgery
Minimally invasive surgery can mean smaller incisional approaches or endoscopic procedures. Using minimally invasive techniques and surgeries provide our patients with many benefits over traditional treatments and surgeries. These benefits typically include:
- Significantly less pain over traditional surgery
- Quicker recovery time
- Faster return to work and normal activities
- Less damage to tissue
- Less scarring
- Outpatient surgery
Endoscopic Decompression of Intermetatarsal Nerve (EDIN) is an endoscopic technique used for Morton’s neuroma treatment. During this technique, two small incisions are made on the foot, one to isolate the ligament and the other for visualization of the ligament via the use of a scope. Once properly visualized, the ligament is cut and this releases the entrapped nerve. This procedure is done in an outpatient setting. Patients are allowed to fully bear weight immediately after surgery as tolerated and return to comfortable shoes the next day. This minimally invasive foot surgery technique allows for faster recovery when compared to the open technique.
Endoscopic Plantar Fasciotomy (EPF) is a minimally invasive, endoscopic technique used to release extreme tension of the plantar fascia. An endoscope provides clear visualization of the inferior surface of the plantar fascia, allowing the surgeon to release tension in the medial band. Following the procedure, a sterile dressing is worn for approximately 3-5 days, then the patient is generally allowed to wear comfortable shoes as tolerated.
Endoscopic Gastrocnemius Recession (EGR) is a minimally invasive technique designed for gastrocnemius equinus treatment. Equinus is a limitation of ankle joint motion. The bi-portal approach, using a scope which provides clear visualization for safe division of the fascia of the gastrocnemius (calf) muscle. The sheath of the scope protects the sural nerve from injury. Once adequate release is attained, all equipment is removed. The skin is closed with sutures. Post-operative management is dependent upon other procedures performed in conjunction with the EGR technique.
Endoscopic Tarsal Tunnel Decompression (ETTD) is a minimally invasive foot surgery technique used to relieve the pressure exerted on the compressed or pinched posterior tibial nerve that runs through the tarsal (Latin term meaning ankle) tunnel on the inner side of the ankle and into the foot. Anything that takes up space in or compresses the tarsal tunnel will put pressure on the nerve and cause numbness, inflammation and pain. This procedure is performed via a small incision determined by anatomic points and geometric lines. The surgery is less traumatic to the patient than an open technique.
Ultrasound guided partial plantar fasciectomy (USGPPF) is a minimally invasive foot surgery technique that uses a high-resolution diagnostic ultrasound to accurately locate and remove the diseased tissue in the plantar fascia and then replace it with growth factors harvested from the patient’s blood. This procedure occurs through a small, needle-like device while the patient is under general anesthesia for a short amount of time. The patient is encouraged to limit the amount of standing or walking for a few days following the procedure. Regular activity is generally resumed within a few days to weeks.
Subtalar Joint Arthroereisis is a minimally invasive flat foot surgery. It is a less aggressive option used to treat a mild or pediatric flatfoot. The implant blocks excessive pronation of the subtalar joint. A small incision is made over the lateral foot, and then a small implant is inserted into the sinus tarsi, a small canal that goes up to the ankle below the talus bone. Minimal dissection allows for a quicker recovery period and a shorter immobilization time when compared to full reconstructive methods.
